Patients that I had treated for well-documented Lyme disease were experiencing chronic joint pain, neurological symptoms and extreme fatigue, yet most lacked “objective measurable manifestations” of Lyme disease, like abnormalities in blood tests or radiologic imaging evidence of tissue damage.Ĭan Lyme disease be a chronic infection? Artur Widak/NurPhoto via Getty Images My training in infectious diseases didn’t prepare me for the patients I started seeing after moving to a Lyme-endemic region in 1996. Without a diagnosis by the establishment, these sick patients are often dismissed and can’t get treated, leading to a sometimes toxic environment as they fight for treatment. These patients are frustrated with a medical establishment whose focus is on evidence-based treatment in a field where evidence is often lacking. The controversy around chronic Lyme disease emerged when patient advocacy groups and some doctors began to use the term to describe patients who had nonspecific symptoms such as fatigue and pain, and testing did not always show that they had been exposed to Lyme disease.Īt the heart of the controversy is the question: Can a person have a chronic bacterial infection that may not show up on tests? Many experts in the field estimate about 10% to 20% of patients diagnosed with Lyme disease get this syndrome. When symptoms linger long after a diagnosed patient receives the standard antibiotic treatment, like the nurse in Maryland experienced, the patient may have a condition called post-treatment Lyme disease syndrome, a subset of chronic Lyme disease. The symptoms can be debilitating, including neurological symptoms, extreme fatigue and muscle and joint pain. The Centers for Disease Control and Prevention now estimates that about 300,000 people in the U.S. Lyme disease, first identified in the United States in the 1970s, has grown into a health epidemic as the ticks that transmit it to humans expand their range. While it may not provide definitive answers yet, we hope it will add to the body of knowledge about this perplexing set of conditions that are likely diverse in origin. Studying this subgroup of post-treatment Lyme disease patients who are treated for Lyme disease but don’t get better is a clue on my way to find to understand chronic Lyme disease. 
Physicians lack the diagnostic tools for early diagnosis or for documenting cure of the disease. Doctors still often don’t know how to accurately diagnose patients with Lyme disease, and patients don’t always get better, even when they are diagnosed and treated. My colleagues and I have closely followed the health of Lyme disease patients as they recover, and what we have discovered runs counter to the mainstream teaching about Lyme disease. 
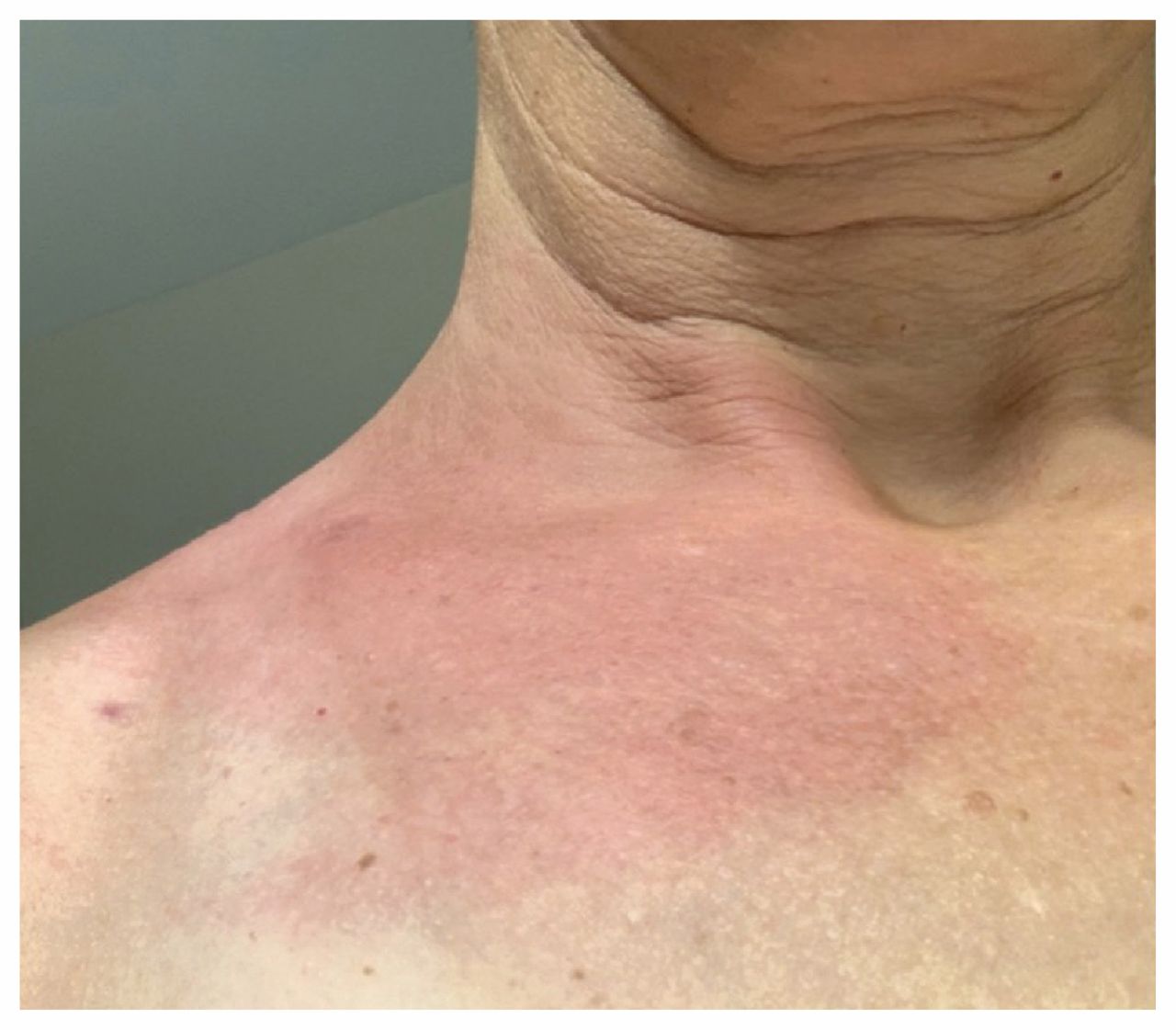
It has become obvious to me that the problem is deeper and more complex than the polarized debate over the controversy would make one believe. Department of Health and Human Services and a medical researcher who has studied chronic Lyme disease for 20 years. I am the former chair of the tick-borne diseases working group at the U.S. Many are denied medications such as antibiotics they believe can control the chronic infections they suspect they have. Her experience gives insight into a highly controversial medical term: chronic Lyme disease.īecause there are no definitive tests or treatments for this condition, patients who have symptoms can be dismissed by the medical establishment. “No one stopped to listen to my story and advocate for me.” “I felt dismissed and abandoned,” she later told me. It wasn’t until several months later, when she got a second opinion, that she was diagnosed with post-treatment Lyme disease, a known complication of Lyme disease. Doctors told her it was just the recovery process, but the symptoms were debilitating and didn’t go away. Doctors tested her for Lyme disease and found it had spread to her heart, a rare manifestation of Lyme disease that can be fatal.Īntibiotics resolved her heart and respiratory symptoms, but the fatigue, as well as joint pain and trouble concentrating, continued. The woman, a nurse in her 40s, returned to the emergency room a few weeks later with breathing trouble and low blood pressure. The next day, she felt worse and went to the emergency room, where she was diagnosed with mononucleosis. Her doctor told her it was likely just a virus. The woman had been healthy until then, and since she enjoyed gardening and landscaping at her rural Maryland home, she wondered if a tick bite might have given her Lyme disease although she had not noticed the telltale bull’s-eye skin lesion. Her symptoms started quickly: neck pain, extreme fatigue and intermittent fever and chills.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
